Medical device and MedTech insights, news, tips and more
Robotic Radical Cystectomy Gaining Momentum as Alternative Open Approach
October 14, 2015
Despite the decline in morbidity and mortality of open radical cystectomy (ORC) during the past two decades, the high rate of perioperative complications remains a challenge for clinicians. After a rocky start with a technically challenging laparoscopic approach, the robot-assisted procedure offered a new horizon.
Expanding on the experience gained with robotic radical prostatectomy, robotic radical cystectomy (RRC) has gained momentum as an alternative to the open approach. Long-term oncologic outcomes with RRC are equivalent to those with ORC.
However, recent prospective data showed that RRC was not superior to ORC in terms of complications and was associated with increased cost. Even though the cystectomy was done robotically, the diversion was performed extracorporeally through an open approach, diluting the advantages of minimally invasive surgery.
Improving RRC Outcomes Through Standardization
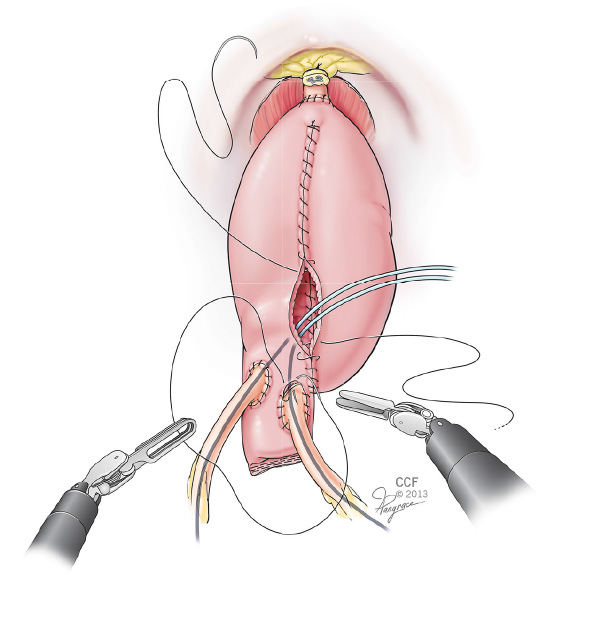
Our experience with RRC and intracorporeal diversion has been encouraging.
Standardizing our technique and defining the steps for intracorporeal ileal conduit and intracorporeal neobladder have allowed us to improve both the intraoperative and postoperative outcomes.
Since the refinement of our technique, we have performed more than 70 RRCs with intracorporeal diversion. The median blood loss for our series is 300 cc. The overall 90 – day complication rate is approximately 50 percent, with a 20 percent rate of high-grade complications (Clavien III/IV) and a 90-day mortality rate of 2 percent. The median time to full diet is 5.5 days, and median hospital stay is seven days.
In comparing the overall cost of our RRCs to ORCs, the overall cost is approximately $2,000 less for the robotic group, despite the higher direct operating room (OR) cost. The lower cost is mainly due to reductions in length of stay and in the rates of major complications and secondary procedures. Although OR time and minor perioperative complications were comparable between RRC and ORC, blood loss, transfusion rate, the rate of major perioperative complications, length of stay and the rate of readmissions were superior with RRC.
By Homayoun Zargar Shostari, MD; Vishnuvardhan Ganesan,BS; and Georges-Pascal
