Medical device and MedTech insights, news, tips and more
Study Links Simulation in EMS Training with Improved Prehospital Pediatric Care
June 24, 2016
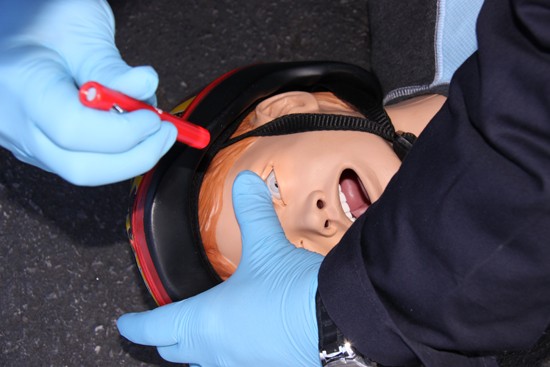
With increased emphasis on culture of safety and rising concerns over medical errors, our attention this month turns to this study from Baylor College of Medicine in conjunction with the Houston Fire Department(HFD).
As we reported in the March issue, we know that the cognitive load theory (CLT) of education impacts high-fidelity simulation in EMS training. Progressive introduction of new materials and effective simulation benefits learners and presumably patient care. Kudos to the authors for taking a scientific approach to measure the effectiveness of simulation and potentially decrease medical errors in high-acuity and low-frequency critical pediatric cases.
To frame this study, it’s important to note that the Agency for Health Care Research and Quality (AHRQ) and the Department of Defense teamed up years ago to implement TeamSTEPPS (www.teamsteppsportal.org), a free educational curriculum introducing culture of safety to healthcare organizations. The authors worked with the HFD and Texas Children’s Hospital to implement a Pediatric Simulation Training for Emergency Prehospital Providers (PediSTEPPs) curriculum and test its effectiveness.
Background: Pediatric patients with high-acuity conditions, such as status-seizures, are as challenging as they are rare for EMS practitioners. This study measured the effects of a high-fidelity simulation training onpediatric seizure protocol compliance by paramedics. The secondary aim of the study was to develop a better understanding of the care EMS and EDs are providing to pediatric seizure patients.
Methods: This was a retrospective cohort study comparing EMS practitioners within the HFD who participated in a specialty simulation training against those who didn’t. PediSTEPPs is a one-day, nine-hour, training that was offered to both BLS and ALS personnel.
The researchers pulled EMS records from a two-year time period for a retrospective review. To meet inclusion criteria, the patients had to be less than 18 years old, actively seizing, cared for by ALS practitioners and transported to an ED. A total of 250 patients met the criteria for inclusion and 65 (26%) of these patients were cared for by a paramedic who had taken a PediSTEPPs course. Protocol compliance was judged by whether the paramedic measured the patient’s blood glucose and administered midazolam to an actively seizing patient.
By
